Click on the link below to see the story Womens Telehealth founders Tanya Mack and C. Anne Patterson, M.D. co-wrote on COVID-19 and Pregnancy beginning on Page 32.
Click on the link below to see the story Womens Telehealth founders Tanya Mack and C. Anne Patterson, M.D. co-wrote on COVID-19 and Pregnancy beginning on Page 32.

Telemedicine — the delivery of healthcare via telecommunication technologies — has been around for decades. But it took an engineer to get it just right.
“We were doing telemedicine at NASA in the early 70’s, but it was completely ‘unsophisticated’ by current standards,” says Georgia Tach aerospace engineering alumna C. Anne Patterson, a board-certified OBGYN and CEO of the Sandy Springs-based Women’s Telehealth.
“We used a satellite to provide information about birth control that people in India could watch in between regular television programing,” remembers Patterson. “I was a propulsion engineer working on that satellite. Later, the satellite was re-purposed to send medical information to physicians in very remote areas of the Rocky Mountains. And that was the extent of our ‘telemedicine’ in the 70s.”
Four decades later, the telemedicine that Patterson now practices is much more than a medically-themed infomercial beamed down from a satellite. It is a systematic use of several technologies (including satellites), all with the goal of delivering personalized medical care directly to patients in remote areas. Telemedicine is also removing one of the largest barriers to health care delivery in the rural South: a chronic shortage of specialized medical practitioners.
“We’ve been able to set up clinics in seven southern states,” says Patterson. “We’ve reached more than 30,000 mostly low-income women — women who would not have access to maternal-fetal health. This is what modern telemedicine is capable of doing.”
Finding her Specialty
Patterson chose her medical specialty — maternal-fetal medicine — in part because it plays such a critical role in Georgia, which has some of the highest rates in the United States for maternal mortality and pre-term delivery, particularly among women of color.
“We conducted a study in Albany Georgia — an area that had preterm birth rates of 18 percent for African-American women, and 16 percent for Hispanic women,” says Patterson. “Those rates were the highest in the state. While it was a tough region to choose, everyone was receptive to trying something new to make a difference.” After bringing telemedicine into the area for 18 months, pre-term birth rates dropped to 8 percent and 6 percent respectively, which is lower than the national average. To date, the rates remain at this level or lower.
Telemedicine is uniquely suited to address the problems faced by the rural poor, Patterson points out. It does not involve high transportation costs, travel time, childcare, or Medicaid. With all of these barriers eliminated, patients are more likely to initiate and maintain contact with the medical system earlier in their pregnancies. Women’s Telehealth helps these high-risk patients to manage chronic health problems — like diabetes and hypertension — that could threaten their pregnancies.
In a typical consultation with Patterson, the conversation rarely ends when doctor and patient have checked off all the obvious medical issues, however. Before the video shuts down, Patterson leans into a more motherly consult with her patients, who have likewise relaxed their once-tense postures. At these moments, it’s a little easier to understand why Patterson is still seeing patients long past the point when most physicians would have retired.
Complete article go to: https://coe.gatech.edu/news/2019/11/engineer-inside-physician
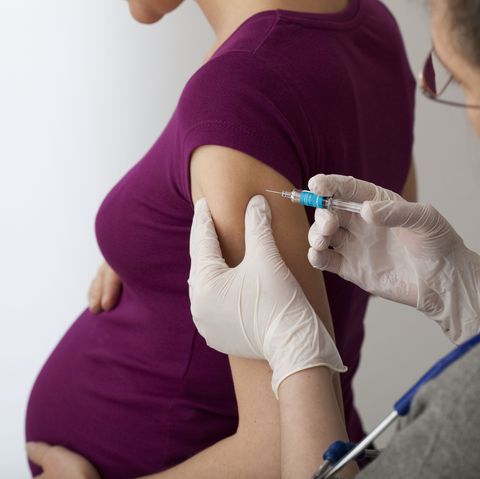
August is National Immunization Awareness Month. It’s a great time for Women’s Telehealth to stress the importance of influenza (flu) vaccination for all moms-to-be, during any trimester. Both the CDC and the American College of Obstetricians and Gynecologists have recommended for years that pregnant women and women who are breastfeeding get the flu vaccine.
Vaccines are made with the highest of safety standards. The influenza vaccine has been proven safe and effective and has not been known to cause pregnancy problems or birth defects. The U.S. FDA approves all vaccines and the CDC monitors all approved vaccines regularly.
Pregnant women are a high risk group for flu due to normal changes in the immune system during pregnancy. Flu is more likely to cause severe illness in pregnant women than in women of reproductive age who are not pregnant. Pregnant women who contract the flu are also at a higher risk for complications of pregnancy such as preterm labor. A 2018 study showed that getting a flu vaccine while pregnant reduced a pregnant women’s risk of getting hospitalized with the flu by 40%.
When pregnant, the flu vaccine does “double duty” by protecting the baby as well. When a pregnant woman gets the flu vaccine, she makes protective antibodies that are transferred to baby. Infants younger than 6 months are at high risk for serious flu-related complications, but once born, are not approved for influenza vaccination until 6 months or older.
Flu vaccines are administered to adults in two ways: injection (shot) into the arm muscle and nasal spray that is inhaled. The shot contains the flu virus in an inactivated form so there’s no risk of it causing the disease. The shot therefore is the recommended form of influenza vaccine during pregnancy. The nasal spray is “live” flu virus and is NOT recommended for pregnant women.
Since the types of virus that can cause flu change, annual flu vaccination is recommended. The side effects of most vaccines are mild and last only a day or two. However, if you have any concerns about side effects after you receive the flu vaccine, consult your obstetrician.
If you are pregnant and think you have the flu, contact your obstetrician right away. Some symptoms of the flu include: fever, chills, body ache, headache, fatigue, cough, sore throat or runny nose. Antiviral medication is available by prescription and has value if taken within 48 hours of the onset of flu. This medicine will not prevent flu. but often shortens the length and severity of flu. You should also contact your obstetrician if you think you may have come in contact with someone who has the flu.
For more information on Pregnancy and Flu visit: https://www.acog.org/Patients/FAQs/The-Flu-Vaccine-and-Pregnancy?IsMobileSet=false or https://www.cdc.gov/flu/highrisk/qa_vacpregnant.htm
Tanya Mack, President
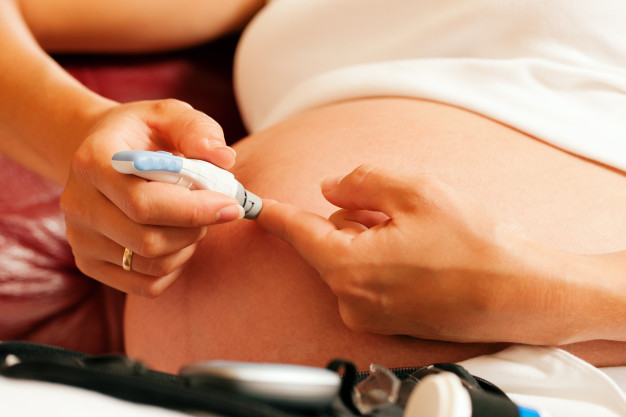
An 18 year old patient presented in a rural area to the local OB physician when she was 16 weeks pregnant. Her OB history showed she had been diagnosed with Type I Diabetes at age 5. She had been seeing a local endocrinologist but was told he would not follow her and manage her insulin during pregnancy.
The close diabetic monitoring required throughout the pregnancy would need to be provided by a Maternal-Fetal Specialist. Because the closest one was approximately 1 ½ hours from the patient’s home, she was referred to Women’s Telehealth by her local OB physician for co-management. Women’s Telehealth provided MFM care through telemedicine visits.
Of additional concern was that the patient was noted to be non-compliant in her insulin regime and diabetic care.
. . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . .
The prevalence of diabetes in pregnancy in the U.S. is increasing. Pre-existing, Type I diabetes confers an increased and more significant risk to both mom and baby than gestational diabetes. Tight blood sugar control is critically important at all stages of pregnancy. Uncontrolled diabetes in pregnancy can lead to such complications as fetal anomalies, pre-eclampsia, fetal demise, macrosomia, neonatal hypoglycemia and spontaneous abortion.
To learn more, visit: https://www.cdc.gov/pregnancy/diabetes-types.html
. . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . .
Our goal in sharing patient case stories is to show the role and possibilities Women’s Telehealth plays in accessing high risk situations and to help turn patient and OB provider concern into the best possible care plans and outcomes for mom’s and their babies. For more information, call our office at: 404.478.3017

This is National Breastfeeding Week in the U.S.! Women’s Telehealth encourages moms to breastfeed, whether you are a first time or experienced mom with a new baby. With that thought in mind, Women’s Telehealth has collected some “Top Tips” to get comfortable with breastfeeding.
For more info on breastfeeding visit: http://peapodnutrition.org/


As part of July Group B Strep Awareness Month, Women’s Telehealth encourages all pregnant women to make sure they complete their Group B Strep testing as part of routine prenatal care.
Group B Streptococcus (GBS) lives in the body naturally and it is a bacteria normally found in 25% of health adult women’s rectum or vagina. Women who test positive for GBS are considered “colonized” or a “carrier.”
GBS is not normally harmful to the mother, but can be harmful to the newborn. A pregnant woman can pass on this infection to the baby during delivery. Not every mom will have symptoms of a GBS infection and not every baby born to a mom with a GBS infection will become ill. While GBS disease can be deadly, there are steps pregnant women can take to help protect their babies.
The CDC recommends all pregnant women get tested for GBS between 35-37 weeks gestation. The most accurate results are within a 5 week period prior to delivery. The rectum and vagina are swabbed during the antepartum OB appointment and the sample is sent to the lab for processing. The results are usually available with a few days.
Rapid screen GBS tests are also available if a woman presents at a facility to deliver and has not had a GBS test completed. If a pregnant woman tests positive, treatment is considered.
Intravenous antibiotics (usually Penicillin for non-allergic patients) are given to women who are at increased risk of having a baby who will develop GBS disease. The antibiotics help protect babies from infection, but only if given during labor. Antibiotics are administered from the onset of labor and continue every 4 hours through to delivery.
The following symptoms may indicate a higher risk of delivering a baby with GBS:
If the baby is delivered via C-section and there is no labor or rupture of membranes, antibiotic treatment is not given. About 1 out of 200 babies of moms with GBS will contract the infection without IV antibiotic treatment. With IV antibiotic treatment, the incidence of babies contracting the infection is lowered to 1 in 4,000.
Early-onset GBS occurs when a baby is infected with GBS within the 1st week of life. Roughly half of babies born with GBS infection have early- onset symptoms including: sepsis, pneumonia, meningitis, breathing problems, heart rate and blood pressure instability and GI and kidney problems. In severe cases, stillbirth may result. Approximately 5% of babies with GBS infections at birth will die.
Late-onset GBS may occur after one week to several months of age. Signs of late-onset GBS include changes in your baby’s eating habits, such as feeding poorly, refusing to eat or not waking for feeding. Changes in baby’s skin, including blue, gray or pale skin due to lack of oxygen, or blotchy or red skin may also be signs of GBS. In the U.S., late-onset GBS has been the leading cause of meningitis in newborns in the first three months of life.
Although research is continuing, there is currently no vaccine for Group B Strep infection. The best two ways to prevent GBS during the first week of a newborn’s life are:
For additional information, please visit:
https://www.cdc.gov/groupbstrep/index.html or https://www.marchofdimes.org/complications/group-b-strep-infection.aspx
Don’t put your un-born baby at risk! Learn the facts and get tested!
~Tanya Mack, President

The US has estimated that 1 million Americans are living with HIV today – and 1 in 7 do not know they have HIV as they have no symptoms. June 27th is World HIV Testing Day and Women’s Telehealth is working to raise awareness about preventing HIV transmission during pregnancy. Prevention starts with HIV testing and knowing your status.
Since 1995, the CDC has recommended that all pregnant women be test for HIV and STD’s in their first and third trimesters and then receive treatment during pregnancy if they test positive for HIV. Yet, recent statistics estimate that in the US, 31% of pregnant women are still not tested for HIV. Concurrent testing for STD’s allows for specifically testing for syphilis (which is treatable) and the prevention of congenital syphilis in the newborn. HIV infection is more prevalent in Southern States, African Americans, and in young people. Testing can be completed in a doctor’s office, hospital, clinic or home.
If the mom’s HIV test is positive or the mom has known HIV infection, with treatment, the risk of transmitting the infection to the newborn can be reduced to approximately 1% through early testing and diagnosis and the use of anti-retroviral therapy (ART) with increasingly effective medicines. The sooner therapy is started the better. The medications work by preventing HIV from multiplying, keeping the viral load in the body low. This helps a pregnant mom stay healthier and significantly decreases the likelihood of transmission during pregnancy or birth. Some of these medications also pass through the placenta adding extra protection for the baby. Most of these ART meds are safe during pregnancy but the best treatment regimen should be determined by a high risk pregnancy specialist.
If pregnant women present to deliver and there are no records of HIV and STD testing, rapid testing prior to delivery can be done with the mother’s consent. If HIV positive moms have a high HIV viral load at the time of delivery, a C-section may be performed to decrease the chance of transmission during the birth process. Babies born to a mom with a known HIV infection will be treated for HIV for 4-6 weeks after birth. To further reduce risk of HIV transmission, HIV positive moms should not breastfeed their newborns.
We are moving in the right direction with preventing transmission during pregnancy through awareness, testing and treatment! From 2012-2016, diagnosed perinatal HIV infections have decrease by 41%! Many states have laws about HIV and STD testing in pregnancy and surveillance upon delivery. For example, Georgia has the HIV and Syphilis Screening Act that mandates all pregnant women be tested for HIV and STD’s in the 1st and 3rd trimester- unless the woman opts out. Also, the law states that if there is no evidence that testing was done prior to delivery when a woman presents for delivery that a rapid HIV screen be performed, unless the mother declines. Similarly, all babies born to an HIV positive mom are required to be reported to the health department within 7 days of birth in GA. Likewise, all babies born with congenital syphilis are to be reported within 24 hours of birth to the local health district officer in the state surveillance system.
HIV transmission to the baby during pregnancy, birth and breastfeeding can be greatly reduced through early testing, treatment and following some precautions. Women’s Telehealth provides high risk pregnancy care via telemedicine – including care of HIV positive moms and their babies – with great results!
Help us raise awareness on World HIV Testing Day by SHARING this blog or checking out further resources:
– For more info, call CDC 800-232-4636
– To schedule HIV testing in your local GA Health Dept., call 800-551-2728
– To find a testing provider nationally, visit: http://www.greaterthan.org or http://www.locator.hiv.gov~Tanya Mack, President

April is Alcohol Awareness Month in the U.S. and a perfect time to raise awareness around prenatal substance abuse and how this affects both the fetus and the newborn. The U.S. has seen a dramatic increase in the past ten years in babies exposed to drugs and alcohol in the womb before birth. Babies that are born to an addicted mother can suffer from withdrawal once born. Babies can’t consciously abstain. We know this and see stories about this in the news every day.
The effects are far reaching and for the baby in utero, may result in low birth weight, slow growth, altered development and in some, lifelong health problems. After the baby is born, Fetal Alcohol Spectrum Disorder (FASD) and Neonatal Abstinence Syndrome (NAS) may require intense intervention in a hospital, perhaps even NICU setting.
Neonates may be exposed to a wide range of substances and it’s hard to know what they may be exposed to due to self-reporting, not knowing the exact components of illicit drugs and wide range of prescription drugs the mother may be taking during pregnancy. All babies do not have withdrawal depending on the length of exposure, the cumulative dose and the baby’s gestational age at birth. Full term babies are more likely to experience withdrawal than preemies.
Symptoms for babies who are experiencing withdrawal often show up within 72 hours of birth, but may not become apparent until a few weeks after delivery. Specific symptoms may vary but include:
Most babies get better initially in 5-30 days and treatments for these conditions include:
As with many health care issues, prevention is preferred over later intervention. Early intervention is a critical path to mitigating problems. Consider:
To help us raise awareness, SHARE THIS MESSAGE to get information into the hands of people dealing with pregnancy and substance abuse.
~Tanya Mack, President
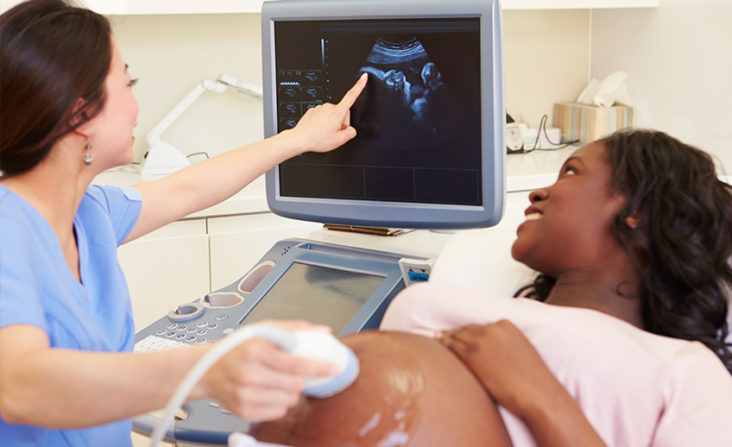
World Prematurity Day is Saturday November 17, a day designed to draw attention to the more than 380,000 babies who are born too soon in the United States every year. Alabama’s pre-term birth rate is 12%, as published in the annual report from the March of Dimes, earning the state a grade of “F” which is unchanged from the previous year. Baptist East Hospital in Montgomery, Women’s Telehealth and Dr. Anne Patterson have launched a new MFM Clinic to support expecting Moms in the prevention of premature births. Please click the link below to view the WSFA news report.

ATLANTA – November 5, 2018 Women’s Telehealth is a recipient of a $5,000 grant in the annual Atlanta Metro Export Challenge (Atlanta MEC), a grant program designed to engage small- and medium-sized businesses in metro Atlanta in the development of international sales plans.
Companies from all over the 29-county region, ranging in size from pre-revenue startups to small and established medium-sized businesses, applied to the program. Thirty companies were selected in the competition and will each receive a grant of $5,000 to apply towards the growth of their international business.
Women’s Telehealth is thrilled to be in receipt of The Atlanta MEC grant and plans to use this funding to make technology enhance to benefit the launch and relationships associated with Project Echo to decrease maternal and infant mortality rates in our partner countries.
Women’s Telehelath provides high risk obstetric service via telemedicine.
To see the full list of grant awardees, click here
The Atlanta MEC is one of many ways to engage small- and medium-sized companies in metro Atlanta in the development of their international business. Over the last two years, the program has given out more than $400,000 to metro Atlanta companies thanks to the generous sponsorship of JPMorgan Chase & Co, which again contributed $100,000 to this year’s program. Additional sponsorship came from the Metro Atlanta Chamber, UPS, Johnson Controls and Partnership Gwinnett.
“JPMorgan Chase is pleased to help metro Atlanta businesses grow in the international economy,” said David Balos, head of JPMorgan Chase’s Middle Market Banking group in Georgia. ‘’These grants will help companies spend time in their target markets to meet with distributors, partners, and potential customers. Seeing metro Atlanta companies grow their international business will consequently lead to job creation and growth of the metro Atlanta economy.”
The Atlanta MEC is being implemented by ORBATL, a regional partnership of metro Atlanta public and private leaders that enables businesses to grow in the global economy through trade and foreign direct investment.