Click on the link below to see the story Womens Telehealth founders Tanya Mack and C. Anne Patterson, M.D. co-wrote on COVID-19 and Pregnancy beginning on Page 32.
Click on the link below to see the story Womens Telehealth founders Tanya Mack and C. Anne Patterson, M.D. co-wrote on COVID-19 and Pregnancy beginning on Page 32.
Listen to the interview with Women’s Telehealth President Tanya Mack as she was a guest on the podcast “Really Know Your Customer”. Click the link below to hear how telemedicine has taken the medical field by storm.

By Tanya Mack, Women’s Telehealth
On March 11th, the World Health Organization declared COVID-19 a worldwide pandemic. As our understanding of COVID-19 expands and our social distancing and separation requirements extend, the need for safe access to care for all, and the protection of pregnant women has become critical. Although we do not yet know if pregnant women have an increased chance of getting sick from COVID-19 compared to the general public, we do know there are changes in their bodies that may increase the risk of infection. We are now seeing indiscriminate and sustained spread across patients in all three trimesters. Within the past month, telehealth has risen to the forefront worldwide as a means to provide quick and safe access to medical care – and the pregnant patient and their obstetric providers are no exception.
Telehealth Enters OB Practice in a Widespread Way
Prior to the COVID-19 pandemic, the use of telehealth was minimal in obstetric practice in the US. Despite its growth in other healthcare areas, few healthcare facilities or providers were set up to provide OB telehealth services. However, in the short span of 4-6 weeks, this has changed dramatically. We have seen ACOG and the Society for Maternal Fetal Medicine (SMFM), hospitals and OB practices quickly respond with broad adoption of telehealth as a means to protect pregnant patients from viral exposure, OB clinical protocols adjusted for telehealth and “pods” of providers during delivery admissions to avoid cross-contamination. As we are learning together, telehealth use can be crucial in meeting healthcare needs during disaster relief.
How Telehealth Works in General and in Obstetrics
Telehealth can be used in many settings such as hospitals, outpatient clinics, doctor’s offices and in patients’ individual homes. Telehealth visits can occur by using satellite, cellular or broadband transmission. Prior to COVID-19, in the US, broadband (internet) was the most common method of transmission. However, cellular transmission is quickly providing access, as it is the most available means for the patient to connect from home via their Smartphone. Clinical standards follow the same guidelines and flow as face-to-face visits. Generally, the connection requirements include: a camera, a microphone and either a cellular or internet connection between the parties.
OB Telehealth visits can occur in the following ways:
Regulatory and Reimbursement Changes in Telehealth During COVID-19 Crisis
Reacting to and being flexible with the current situation, the federal government has greatly relaxed prior barriers to telehealth in recent weeks. Although few pregnant patients have Medicare as a payor, the Centers for Medicare and Medicaid Services (CMS) has set standards that many state Medicaid and commercial carriers are following as well. Some of these temporarily “relaxed” guidelines for telehealth use and payment during this crisis are:
For reimbursement, although CMS and Medicare have lifted restrictions for payment nationwide and temporarily, each state controls their Medicaid coverage and each commercial healthcare payer determines their telehealth coverage. Patients are encouraged to follow and check with their own carrier and state, but an overwhelming majority are covering telehealth during this public health emergency. In general, although the use of telehealth and reimbursement for it are changing daily, preventing the spread of COVID-19 in pregnant patients remains the #1 priority in obstetrics.
Obstetric Protocol Adjustments for Low and High-Risk OB Patients Using Telehealth
Obstetric professional organizations such as delivering hospitals, ACOG and SMFM are adapting clinical guidelines for telehealth. The idea is to have OB patients come in for critical antenatal appointments such as the 11-13 weeks dating scan and labs, 20-week anatomy ultrasound, and the 26-18 week GTT testing and end of pregnancy visits. Telehealth antenatal visits can be used for <11 weeks initial assessment visits, blood pressure checks for pre-eclampsia and glucose monitoring for gestational diabetes, and kick counts/telehealth follow-up versus in-person nonstress tests (NSTs), etc.
As there is no vaccine for COVID-19 yet, limiting risk for pregnant patients during this pandemic remains a priority. Worldwide organizations are sharing COVID-19 pregnancy information at a rate we’ve never seen before, to ascertain how the virus affects mom and the fetus, whether vertical transmission occurs between mother and fetus, what treatments are effective and more. In the interim, the benefits of using telemedicine in obstetrics are clear. Telemedicine provides easier access to specialty care, is consistent with the social distancing policies, is often cheaper than an in-person visit, and decreases unnecessary travel.
Prior to the COVID-19 pandemic, Women’s Telehealth provided over 34,000 high-risk OB visits 100% by telehealth. As providers and patients grow accustomed to using this modality in obstetrics, many for the first time, Women’s Telehealth is available to help. Contact Tanya Mack, Women’s Telehealth, 404-478-3017 or visit www.womenstelehealth.com.
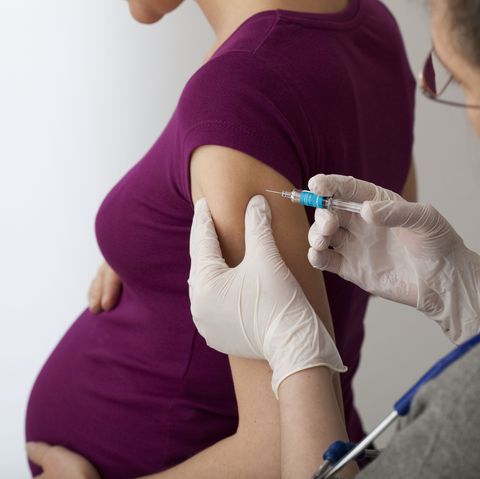
August is National Immunization Awareness Month. It’s a great time for Women’s Telehealth to stress the importance of influenza (flu) vaccination for all moms-to-be, during any trimester. Both the CDC and the American College of Obstetricians and Gynecologists have recommended for years that pregnant women and women who are breastfeeding get the flu vaccine.
Vaccines are made with the highest of safety standards. The influenza vaccine has been proven safe and effective and has not been known to cause pregnancy problems or birth defects. The U.S. FDA approves all vaccines and the CDC monitors all approved vaccines regularly.
Pregnant women are a high risk group for flu due to normal changes in the immune system during pregnancy. Flu is more likely to cause severe illness in pregnant women than in women of reproductive age who are not pregnant. Pregnant women who contract the flu are also at a higher risk for complications of pregnancy such as preterm labor. A 2018 study showed that getting a flu vaccine while pregnant reduced a pregnant women’s risk of getting hospitalized with the flu by 40%.
When pregnant, the flu vaccine does “double duty” by protecting the baby as well. When a pregnant woman gets the flu vaccine, she makes protective antibodies that are transferred to baby. Infants younger than 6 months are at high risk for serious flu-related complications, but once born, are not approved for influenza vaccination until 6 months or older.
Flu vaccines are administered to adults in two ways: injection (shot) into the arm muscle and nasal spray that is inhaled. The shot contains the flu virus in an inactivated form so there’s no risk of it causing the disease. The shot therefore is the recommended form of influenza vaccine during pregnancy. The nasal spray is “live” flu virus and is NOT recommended for pregnant women.
Since the types of virus that can cause flu change, annual flu vaccination is recommended. The side effects of most vaccines are mild and last only a day or two. However, if you have any concerns about side effects after you receive the flu vaccine, consult your obstetrician.
If you are pregnant and think you have the flu, contact your obstetrician right away. Some symptoms of the flu include: fever, chills, body ache, headache, fatigue, cough, sore throat or runny nose. Antiviral medication is available by prescription and has value if taken within 48 hours of the onset of flu. This medicine will not prevent flu. but often shortens the length and severity of flu. You should also contact your obstetrician if you think you may have come in contact with someone who has the flu.
For more information on Pregnancy and Flu visit: https://www.acog.org/Patients/FAQs/The-Flu-Vaccine-and-Pregnancy?IsMobileSet=false or https://www.cdc.gov/flu/highrisk/qa_vacpregnant.htm
Tanya Mack, President
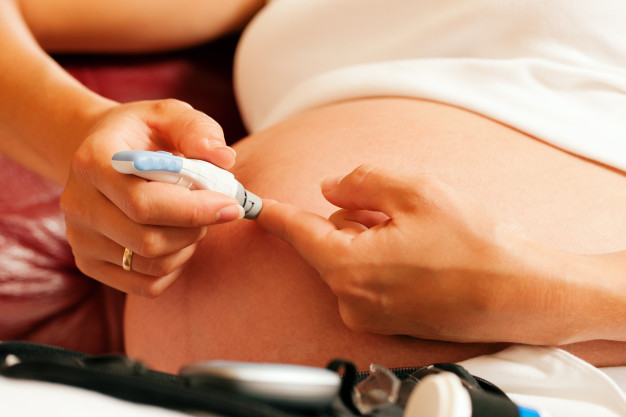
An 18 year old patient presented in a rural area to the local OB physician when she was 16 weeks pregnant. Her OB history showed she had been diagnosed with Type I Diabetes at age 5. She had been seeing a local endocrinologist but was told he would not follow her and manage her insulin during pregnancy.
The close diabetic monitoring required throughout the pregnancy would need to be provided by a Maternal-Fetal Specialist. Because the closest one was approximately 1 ½ hours from the patient’s home, she was referred to Women’s Telehealth by her local OB physician for co-management. Women’s Telehealth provided MFM care through telemedicine visits.
Of additional concern was that the patient was noted to be non-compliant in her insulin regime and diabetic care.
. . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . .
The prevalence of diabetes in pregnancy in the U.S. is increasing. Pre-existing, Type I diabetes confers an increased and more significant risk to both mom and baby than gestational diabetes. Tight blood sugar control is critically important at all stages of pregnancy. Uncontrolled diabetes in pregnancy can lead to such complications as fetal anomalies, pre-eclampsia, fetal demise, macrosomia, neonatal hypoglycemia and spontaneous abortion.
To learn more, visit: https://www.cdc.gov/pregnancy/diabetes-types.html
. . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . .
Our goal in sharing patient case stories is to show the role and possibilities Women’s Telehealth plays in accessing high risk situations and to help turn patient and OB provider concern into the best possible care plans and outcomes for mom’s and their babies. For more information, call our office at: 404.478.3017
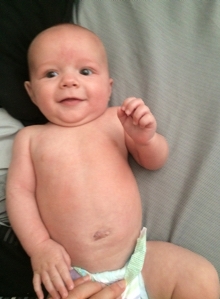
How to successfully manage the complexities of gastroschisis in pregnancy is the focus of this Women’s Telehealth patient story. [Pictured above: Gastroschisis Baby – Post Op]
At the anatomy ultrasound scan at 17 weeks, the OB physician found that his 24 year old Caucasian patient had a suspected gastroschisis.
Gastroschisis is a birth defect in which the fetus’ intestines and/or stomach protrude outside the abdominal wall. A baby with this condition requires immediate surgery after birth to place the organs in the proper place in the abdominal cavity and close the hole in the abdominal wall. Hospitalization is also needed for an extended period of time to ensure that the baby’s feeding and digestive tract are functioning well. Most babies with appropriate care and surgery at birth will grow up to have normal lives. Successful outcomes often depend on early identification of this birth defect and preparing for surgery upon birth.
In addition to the suspected gastroschisis, other complicating factors included mom’s obesity, pregnancy-induced hypertension, low amniotic fluid, abnormal cervix and active kidney disease. The mom-to-be also needed an extra dose of oversight and compassion due to the loss of a baby during a previous pregnancy, caused by open neural tube defect.
The mom-to-be was referred by the OB physician to Women’s Telehealth maternal-fetal medicine (MFM) physicians for diagnosis and collaborative pregnancy management. Women’s Telehealth was asked to manage BOTH infant and maternal pregnancy complications.
. . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . .
The CDC estimates that Gastroschisis affects 1 in every 1,900 babies born in the U.S. each year. The cause of this birth defect is currently unknown but researchers have speculated that potential causes may be adaptations in genes and/or the lifestyle or environment of the mother. Young, Caucasian women are the most common population to be at risk. For more information about this condition visit: https://www.cdc.gov/ncbddd/birthdefects/gastroschisis.html
. . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . .
WT partners with OB/GYN physicians and healthcare facilities to provide the highest level of Maternal-Fetal Medicine (MFM) available through telemedicine. WT provides services in local hospitals, doctor’s offices and government clinics.
Our goal in sharing patient case stories is to show the role and possibilities Women’s Telehealth plays in accessing high risk situations and to help turn patient and OB provider concern into the best possible care plans and outcomes for moms and their babies. For more information, call our office at: 404.478.3017

This is National Breastfeeding Week in the U.S.! Women’s Telehealth encourages moms to breastfeed, whether you are a first time or experienced mom with a new baby. With that thought in mind, Women’s Telehealth has collected some “Top Tips” to get comfortable with breastfeeding.
For more info on breastfeeding visit: http://peapodnutrition.org/


Women’s Telehealth and Eagle Telemedicine are working together to bring scarce, high risk OB services to more communities across the country!
Eagle Telemedicine is a premier telemedicine organization with a national network that brings a wide variety of healthcare providers to acute and critical access hospitals and health organizations. They provide night coverage and specialty care as well as fill staffing gaps, all exclusively by telemedicine. Eagle Telemedicine provides over 20,000 telemedicine patient encounters annually. Women’s Telehealth has completed over 31,000 maternal fetal medicine patient encounters/studies.
“This alliance will expand the capabilities of both companies,” said Women’s Telehealth President, Tanya Mack. “Eagle Telemedicine now adds maternal-fetal medicine to their service line and Women’s Telehealth gains expanded geographic coverage.” Builders and shapers in their respective areas of the telemedicine industry, the companies share mutual goals of bringing much needed specialty care to where it is needed and serving the underserved in a sustainable, cost effective manner. The companies’ combined strengths will allow high risk moms to keep their care local and allow hospitals and healthcare organizations to retain their patients and provide scarce specialty care.
For more information visit:
http://: https://www.eagletelemedicine.com/telemedicine-services/telespecialty-services/telematernal-fetal-services/

As part of July Group B Strep Awareness Month, Women’s Telehealth encourages all pregnant women to make sure they complete their Group B Strep testing as part of routine prenatal care.
Group B Streptococcus (GBS) lives in the body naturally and it is a bacteria normally found in 25% of health adult women’s rectum or vagina. Women who test positive for GBS are considered “colonized” or a “carrier.”
GBS is not normally harmful to the mother, but can be harmful to the newborn. A pregnant woman can pass on this infection to the baby during delivery. Not every mom will have symptoms of a GBS infection and not every baby born to a mom with a GBS infection will become ill. While GBS disease can be deadly, there are steps pregnant women can take to help protect their babies.
The CDC recommends all pregnant women get tested for GBS between 35-37 weeks gestation. The most accurate results are within a 5 week period prior to delivery. The rectum and vagina are swabbed during the antepartum OB appointment and the sample is sent to the lab for processing. The results are usually available with a few days.
Rapid screen GBS tests are also available if a woman presents at a facility to deliver and has not had a GBS test completed. If a pregnant woman tests positive, treatment is considered.
Intravenous antibiotics (usually Penicillin for non-allergic patients) are given to women who are at increased risk of having a baby who will develop GBS disease. The antibiotics help protect babies from infection, but only if given during labor. Antibiotics are administered from the onset of labor and continue every 4 hours through to delivery.
The following symptoms may indicate a higher risk of delivering a baby with GBS:
If the baby is delivered via C-section and there is no labor or rupture of membranes, antibiotic treatment is not given. About 1 out of 200 babies of moms with GBS will contract the infection without IV antibiotic treatment. With IV antibiotic treatment, the incidence of babies contracting the infection is lowered to 1 in 4,000.
Early-onset GBS occurs when a baby is infected with GBS within the 1st week of life. Roughly half of babies born with GBS infection have early- onset symptoms including: sepsis, pneumonia, meningitis, breathing problems, heart rate and blood pressure instability and GI and kidney problems. In severe cases, stillbirth may result. Approximately 5% of babies with GBS infections at birth will die.
Late-onset GBS may occur after one week to several months of age. Signs of late-onset GBS include changes in your baby’s eating habits, such as feeding poorly, refusing to eat or not waking for feeding. Changes in baby’s skin, including blue, gray or pale skin due to lack of oxygen, or blotchy or red skin may also be signs of GBS. In the U.S., late-onset GBS has been the leading cause of meningitis in newborns in the first three months of life.
Although research is continuing, there is currently no vaccine for Group B Strep infection. The best two ways to prevent GBS during the first week of a newborn’s life are:
For additional information, please visit:
https://www.cdc.gov/groupbstrep/index.html or https://www.marchofdimes.org/complications/group-b-strep-infection.aspx
Don’t put your un-born baby at risk! Learn the facts and get tested!
~Tanya Mack, President

Virtual pregnancy care spans from prenatal to postpartum care. It incorporates a variety of telehealth modalities including audiovisual visits, remote patient monitoring and “live” and asynchronous store and forward imaging.
The Advisory Board is the best practice firm helping healthcare organizations worldwide improve their performance using a combination of research, technology and consulting. They have 12 offices on 3 continents and publish to over 9,000 healthcare organization outlets.
Recently, the Advisory Board published the piece, “Telehealth Primer: Pregnancy Care.” The publication features four innovative healthcare organizations using telehealth tools to deliver different aspects of pregnancy care and their business cases and results.
Women’s Telehealth is pleased to be featured in the primer for our work in providing maternal-fetal medicine services, delivered 100% via telemedicine, to help decrease preterm labor and improve access to maternal-fetal medicine providers.
The Mayo Clinic’s OB Nest program and the University of Utah were also featured in the Primer for their work in delivering antepartum visits virtually vs. in-person visits, to improve patient satisfaction with the same clinical outcomes.
The Primer also featured the University of Pennsylvania for delivering postpartum visits via remote patient monitoring to ease post-delivery care and outcomes for new moms.
For a copy of this informative primer, visit: https://www.advisory.com/research/service-line-strategy-advisor/resources/2018/telehealth-primer-pregnancy-care